Red skin
We’ve all had red skin at some point in our lives. Temporary redness can come from embarrassment (blushing) or a menopausal hot flush. However, more lasting redness can be due to a range of reasons including sunburn or a reaction to alcohol, as well various skin conditions. This redness, known as erythema, can be caused by dry or sensitive skin. It can also be due to an underlying skin condition such as eczema or contact dermatitis – or an infection.
You’ll probably find that you have other symptoms alongside the redness, acting as clues to help you, or your healthcare practitioner, identify what the problem is.
Symptoms associated with red skin
- Itchy skin
- Flaky skin
- Red skin
- Inflamed skin
- Blisters/ pustules
- Hives/urticaria
- Bumpy skin
- Dryness
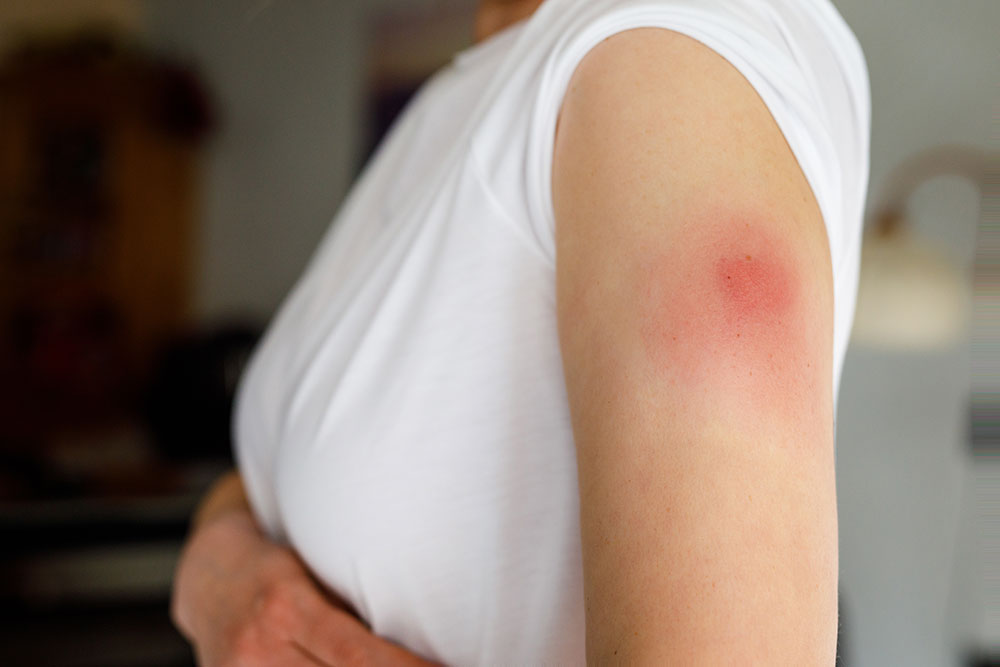
Conditions linked to red skin
The reason for skin redness is sometimes obvious but on other occasions, it might be less clear. It might be because you have dry skin, it could be a reaction to an allergen or irritant and/or due to a skin infection.
Dry skin
Dry skin develops if you don’t have enough moisture or oils in your skin. Although it’s more common in older people, anyone can develop dry skin as a reaction to our environment, the clothes we wear and everyday products that we use. Mild dry skin may not cause any redness at all, but it’s with more severe dry skin that some redness can appear.
Eczema
Eczema is a dry, inflammatory skin condition. If you have eczema your skin may not produce as much fat and oils as normal skin, which means it doesn’t trap moisture as effectively. There are different types of eczema, many of which have red skin as a symptom. These include:
- Atopic eczema – which usually starts in childhood, though up to 1 in 10 adults also develop the condition. It’s more common if you have asthma and/or hayfever
- Contact dermatitis – a type of eczema caused by your skin coming into contact with an allergen or irritant. If you have the type of job where you are exposed to allergens and irritants regularly – for example hairdresser, cleaner or bar worker – then you’re more prone to developing contact dermatitis
- Seborrhoeic eczema – this is better known as cradle cap in babies and dandruff in adults, where men are at slightly more increased risk.
Infections
Skin infections can be caused by fungi and yeasts, bacteria and viruses. Obviously, there are many, many different organisms that can cause problems but some of the more common skin infections are:
- Fungal skin infections. Athlete’s foot or ringworm are both caused by a type of fungus called a dermatophyte. Around 70% of us have athlete’s foot at some point in our lives, particularly as teenagers. Most people with athlete’s foot have white or red skin with scaly or moist skin between the toes, usually between the two smallest toes
- Bacterial skin infections. In addition to causing red skin, bacterial skin infections can also make your skin feel hot and swollen, and you may develop lumps or abscesses. While most bacterial skin infections clear up on their own or with antibiotics, some can be serious if not treated quickly – like cellulitis
- Viral skin infections. There are many viral skin infections, but one thing a lot of them have in common is a red rash. This can be due to common childhood conditions, such as measles or chickenpox, and will be accompanied by other symptoms such as fever, tiredness and headache.
Psoriasis
The most common type of psoriasis is plaque psoriasis, where there are pink-red patches of skin covered in silver-white scales – particularly on the limbs, trunk and scalp. Psoriasis develops when the rate at which our skin cells are renewed happens much faster than normal. There are times when psoriasis can flare up and your skin is more irritated than usual – for example after an infection, from exposure to intense sunlight or because of stress.
Rosacea
Rosacea is an incurable skin problem that affects people with fair skin, usually between the ages of 40 and 60. Although you’re more likely to develop the condition if you’re a woman, men tend to have worse symptoms. Rosacea usually affects the face and the first sign can be that you blush more easily than normal. Over time, your cheeks, chin, forehead and nose change colour to become a darker red. You’ll also notice the blood vessels in these areas become dilated and your skin develops pustules and bumps, which looks like acne. Some people find the skin around their eyes also becomes swollen or their nose gets enlarged – more commonly in men. It’s not really known what causes rosacea but it could be a mix of environmental factors, genetics and your immune system.
Urticaria
Urticaria, also known as nettle rash or hives, tends to affect people between the ages of 20 and 40 and is more common in women. It happens when chemicals, such as histamine, are released in the skin – causing a red, raised itchy rash. Urticaria can occur after a viral infection, particularly in children. It can also develop if you have an allergic reaction to food – for example peanuts, shellfish, milk and eggs – or insect bites, medicines like penicillin, and latex. For some people, it can just be triggered by coming into contact with sunlight, cold, heat or water.
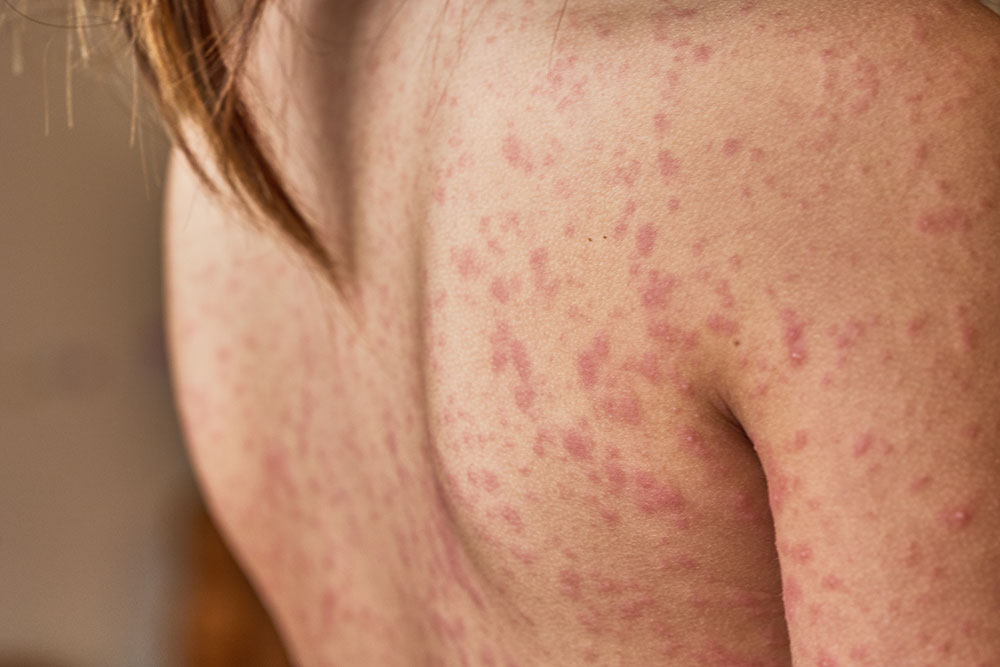
Red skin triggers and factors
Although there are many things that can make our skin go red – from what we eat and what we wear to our lifestyle – it might take some time figuring out the specific cause in each case.
Allergens and irritants
Allergens and irritants can cause red skin reactions. House-dust mites, pollen, pet dander, perfume, cosmetics, hair dyes, metals such as nickel, medicines and plants can all be common culprits.
How to manage:
- If you can, try to avoid the allergen or irritant
- If you can’t avoid it, wash it off as soon as you can after touching and ideally, use an emollient soap substitute
- When you’re dusting, wipe with a damp cloth rather than a duster (this can spread allergens into the air)
- Use unscented products, including skincare, as much as possible
- Antihistamines can help you keep your allergies under control.
Cleansers
Soaps and cleansers are detergents which can remove vital water and fats from our skin, making the skin barrier less robust. If you have dry skin, eczema, contact dermatitis or rosacea, cleansers can irritate your skin, making it worse.
How to manage:
- Use an emollient soap substitute to wash instead of soap
- Swap long, hot baths for short baths or showers with luke-warm water (10 minutes maximum)
- Steer clear of perfumed products
- If you have rosacea, don’t scrub your skin when washing your face
- Use cotton-lined gloves when washing up
- Take off any rings before you wash your hands to stop soap from collecting underneath
- To keep your clothes irritant-free, rinse them twice when washing and consider using fabric balls instead of detergent.
Sweat
Some people with eczema or rosacea can find that sweating makes their condition worse. That’s because as we sweat, we lose water from the skin and sodium in our sweat can irritate the skin surface.
How to manage:
- Exercise that makes you sweat can make rosacea and eczema worse, so try gentle rather than intense exercises
- Drink water and moisturise before and after exercise to stay hydrated
- Wear the right clothes – tight, synthetic fibres can irritate, so choose loose, natural fabrics instead
- It’s okay to take breaks – in fact, it’s encouraged
- Cold pads can help cool your skin
- Shower daily, especially after a workout to rinse off any sweat and avoid irritating skin further,
Food
Some foods can cause urticaria and irritant contact dermatitis, causing redness. Others can make rosacea worse.
How to manage:
Avoid foods that trigger a reaction as much as possible – you might find it helpful to keep a food diary to help you identify the culprit If you have rosacea, alcohol, hot drinks and spicy foods can be particularly irritable for your skin Wear cotton-lined gloves and wash with soap substitute before and after food preparation.
Stress
Our body’s natural response to stress is to release certain chemicals to help it cope. However, these can have a negative effect on our skin – making dry skin, eczema, psoriasis and rosacea worse.
How to manage:
- Try relaxation techniques, like deep breathing, mediation, yoga or tai chi
- Distract yourself from your stress by doing something more relaxing instead – like baking, knitting, writing or painting
- Get a good night’s sleep if you can
- Exercise is always good, so make sure it becomes a regular thing for you
- If you find that you’re struggling to manage your stress, contact a healthcare professional for advice.
Weather and temperature
Anything that reduces humidity – such as air conditioning, central heating or wood burners – can make your skin dry, leading to redness. As a result, dry skin, eczema and psoriasis are worse in the winter.
How to manage:
- Keep your house at the ideal temperate of 18°C
- Extremes of temperature also make rosacea worse
- If you want to increase the humidity in your home, use a humidifier or place bowls of water under radiators
- Avoid convection heaters, if you can
- Your rosacea can be sensitive to the sun, so always make sure you wear a sunblock of at least SPF 30 to protect your skin.
How to manage red skin
Finding out what’s causing your red skin can help you manage it better. There’s a big difference between treating eczema and treating a fungal infection, for example. There are many different treatments available that can help ease red skin depending on the cause.
Emollients
If dry skin, eczema, contact dermatitis or psoriasis are the underlying cause of your redness, then using an emollient regularly can help. Emollients are moisturisers which should be applied often everyday – at least twice a day. Always use generous amounts, even when you feel your skin doesn’t need them. However, always read and follow the instructions on the emollient you are about to use, unless told to otherwise by your doctor.
Applying emollients regularly can help soothe red skin by:
- Adding moisture to skin and trapping it inside
- Forming a protective barrier over the skin to keep irritants out
- Helping flare ups of conditions, such as eczema.
Washing with an emollient or soap substitute is also recommended as regular soaps and cleansers can irritate the skin and cause further dryness. Emollients don’t foam up like soaps, but they still work to get you clean. If you’re having a bath, you can also add emollient bath oils.
Steroids
Mild steroid creams and ointments can be bought from your pharmacy to help relieve contact dermatitis and mild-to-moderate eczema – helping to reduce redness. These types of creams can also help with insect bites and certain forms of allergies; please always read the label to ensure you are using the steroid product correctly and for the right thing. If in doubt, talk to a healthcare practitioner.
It’s important to know that majority of steroid creams are applied very differently to emollients:
- Apply very thinly and to just a small area
- Apply once or twice a day for a maximum of 7 days (always check the label of your product)
- Only apply to certain parts of the body and not to the face, eyes, broken or infected skin, genital areas or the bottom
- Majority have age restrictions so please check the label
- If you are pregnant or breastfeeding, you should speak to your doctor before using a steroid cream.
If your redness is still there after a week, see your doctor as you may need a different treatment.
Antihistamines
Antihistamines can be used to help relieve certain conditions such as atopic eczema, contact dermatitis and urticaria. Ask your pharmacist or doctor for advice on taking an antihistamine that’s right for you.
Antifungals
Antifungal creams and ointments are available to treat athlete’s foot and ringworm. Some also contain a mild steroid to help reduce any inflammation. Consult with your pharmacist before use to ensure the product is correct for your situation.
Speak to your doctor or pharmacist if:
- Self-care treatment has not worked after a week
- If the redness is getting worse or the red area is growing bigger very quickly
- The red area is hot, swollen, painful or blistered
- You also feel unwell
- If there is a rash that doesn’t fade when you press a glass against the skin.
Self-Care for red skin
Self-care can include avoiding triggers, using emollients daily to manage dry skin and taking care with your lifestyle choices.
Do
- Use an emollient moisturiser daily and regularly
- Take care when choosing clothing and fabrics
- Protect skin appropriately; this can include sunscreen
- Switch from soap to a non-soapy emollient cleanser
- Keep showers short and use tepid or cool water
- Use cool pads as a soothing compress.
Don’t
- Eat foods that can cause an allergic reaction – such as shellfish or dairy products – or that make rosacea worse, for example alcohol, hot drinks and spicy foods
- Scratch skin
- Have long, hot baths or showers
- Expose skin to extreme temperatures
- Expose skin to known irritants or allergens.
No products found